Quality Improvement Program
Read the Magazine in PDF
Abstract
The article discusses applying quality improvement programs in the public health sector and their relevance in various work environments. It distinguishes between quality improvement programs and individual projects, highlighting six dimensions of healthcare quality for high standards. Principles for successful quality improvement programs are outlined, including Juran’s trilogy and the significance of QI models.
Introduction
Quality improvement programs are essential not only in healthcare settings but also in the public health domain. The course imparts fundamental principles applicable to any work environment, covering intricate quality management structures and successful program development. Participants gain skills to establish effective quality improvement programs in their workplace.
Quality improvement programme
To address quality improvement programs effectively, it’s important to differentiate them from tasks, activities, and projects. These programs aim to close performance gaps and enhance healthcare quality. A shared understanding of quality is vital before starting such programs. The Institute of Medicine defines quality as improving health outcomes in line with professional knowledge. The World Health Organization emphasizes quality healthcare for universal coverage and better outcomes. Quality-of-care is determined by its impact on health outcomes and alignment with recognized dimensions by both organizations.
Hacking the QIP Code
Quality improvement programs are not based on random results but are specifically designed to produce desired outcomes. In order for a quality improvement program to be successful, there are certain principles that must be followed, which are as follows;
- Setting and meeting relevant and significant standards: Reaching a consensus on quality benchmarks is crucial, but knowing the standards alone isn’t enough for desired outcomes.
- Building infrastructure informed by the standard you’ve set: Patients and clients should be considered when building this infrastructure, not just in the hospital or diagnostic space, but also in public health as a whole.
- Data-driven quality improvement: Organizations must have the ability to collect and use robust, relevant, and quality data.
- Accountability: It is critical to the success of a quality improvement program. Regular external verification helps keep organizations on their toes and ensures a system of accountability that helps continually improve the system.
The Six Dimensions of Health
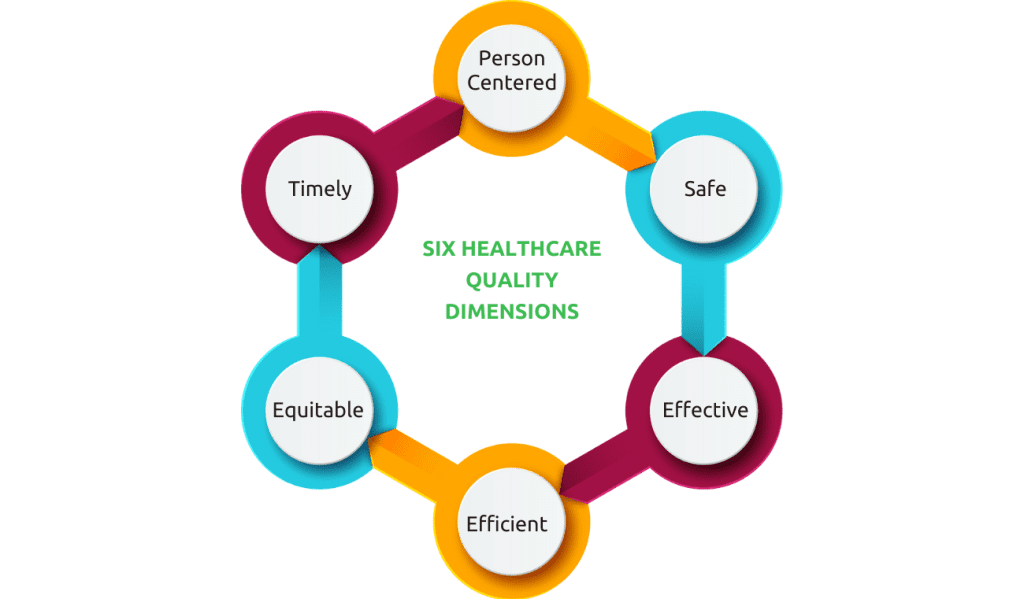
The Institute of Medicine and the World Health Organization identifies the STEEEP aspects for high-quality healthcare: safe, effective, efficient, equitable, and timely, with person-centered care. These dimensions form a framework to assess and improve healthcare delivery, prioritizing the individual or population being served in all decisions and design considerations.
Quality AcJuran’s Trilogy
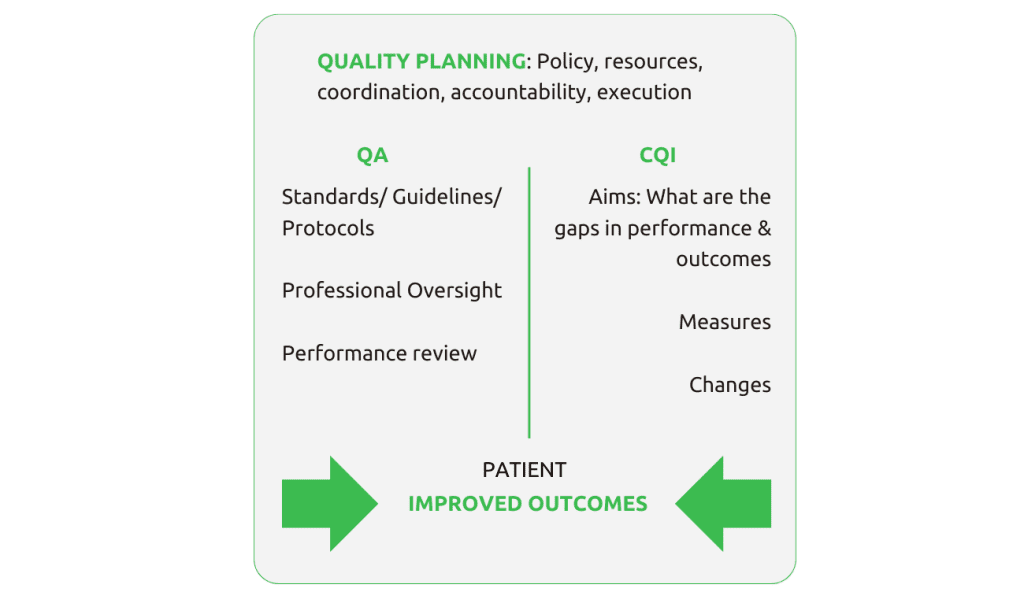
Joseph Duran proposed a three-component quality management system, which includes;
- Quality planning,
- Quality control/assurance, and
- Quality improvement.

The quality planning component involves setting up the necessary environment for organizations to succeed, including
- Establishing processes,
- Policies,
- Governance, and
- Coordination
Quality planning, control/assurance, and improvement are crucial elements in any system, be it a hospital, lab, or country. Quality planning establishes objectives and allocates resources, while quality control ensures adherence to standards and performance evaluation. Quality improvement closes the gap between present and desired performance, using feedback and continuous strategies.
When a system operates at 40% capacity, unexpected events like COVID-19 can cause a drop to 20%, leading to chaos and burnout. Introducing a quality improvement program can restore performance to 80-85% and stabilize it. Continuous improvement prevents future anomalies, enhancing effectiveness, efficiency, and productivity, even though zero harm and perfection are unattainable in healthcare.
Why QI models?
Frameworks and models offer guidance, structure, and a roadmap for organizing improvement initiatives in organizations. They help with planning, resource management, and teamwork, empowering action and iterative learning. Without a model, clarity on roles and responsibilities may suffer.
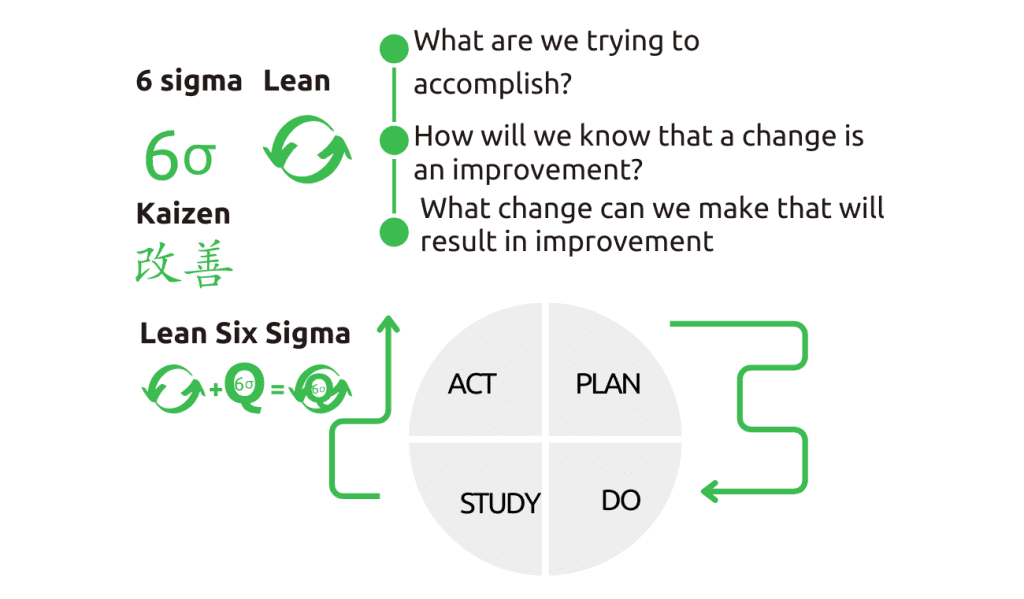
Common quality improvement models in healthcare include Six Sigma, Lean Six Sigma, Kaizen, 5S, and the Model for Improvement (also known as “Favors” in the HIV field). These models foster a shift from random activities to systematic and methodical approaches for enhancing healthcare.
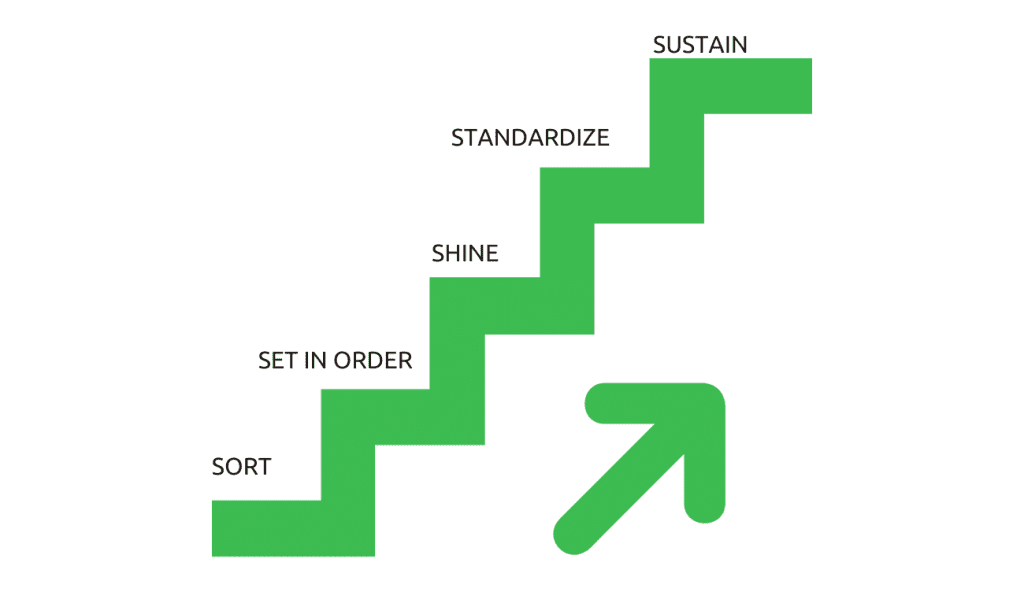
The 5S Kaizen
During a visit to a rural Ethiopian delivery room, the lack of organization caused delays in care. Implementing the 5S Kaizen approach, with its five steps: sort, set in order, shine, standardize, and sustain, was suggested. Creating an emergency trolley with easily accessible equipment would improve efficiency and care. Playing a game can demonstrate the approach’s benefits, reducing costs, enhancing productivity, and ensuring a safer work environment. By adopting a well-organized and Kaizen-compliant workspace, resources are used efficiently, and work processes are streamlined for improvement.
The Model for Improvement
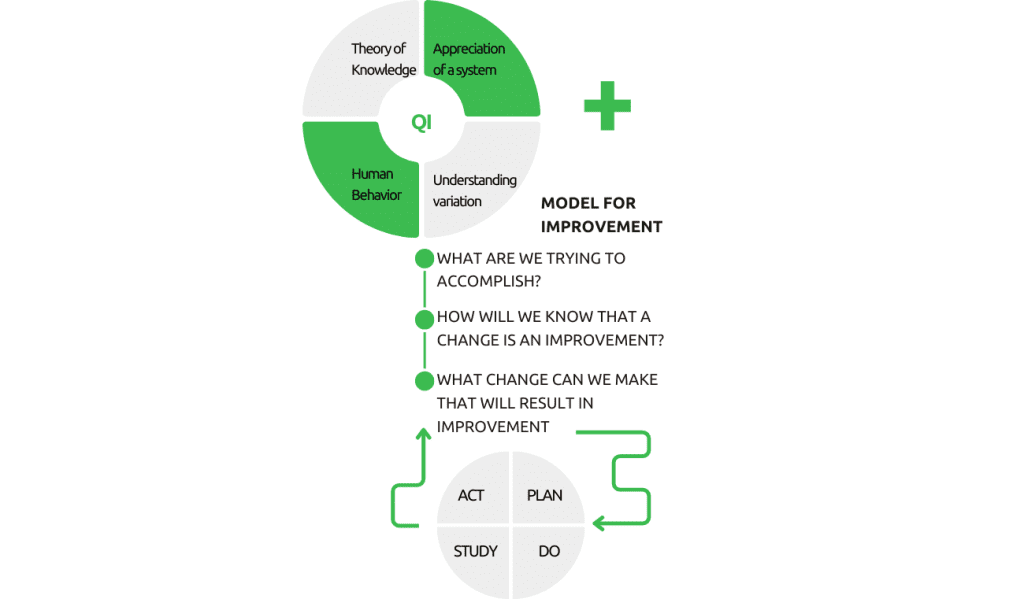
The Model for Improvement involves three questions, PDSA cycles, and measurements to gauge progress.
- The first question sets aim and identifies responsible parties.
- The second question focuses on outcome, process, and balancing measures.
- The third question emphasizes testing changes with the PDSA cycle to ensure improvement.
This approach helps identify effective changes for improvement.
How to create an effective QIP?
To create an effective Quality Improvement Program, follow these steps: establish the “why,” define quality, prioritize improvement areas, collect and analyze data, develop a tailored model, leverage system knowledge, and commit to ongoing evaluation and transparent communication. Integrating the “System of Profound Knowledge” with other improvement models like MFI or Lean Six Sigma enhances success. Understand systems thinking, theory of knowledge, variation, and the psychology of change for impactful implementation. By embracing these processes and principles, your quality improvement program can surpass expectations and achieve meaningful results.
DEMING’S SYSTEM OF PROFOUND KNOWLEDGE
Conclusion
A Quality Improvement Program is vital in healthcare and beyond, involving systematic activities to monitor and enhance healthcare quality. It adheres to six dimensions: safe, effective, efficient, equitable, timely, and person-centered care. Guided by principles and models like Juran’s Trilogy, it sets relevant standards, utilizes data-driven improvement, and ensures accountability. Implementing this program improves organizations’ effectiveness, efficiency, and productivity, benefiting the patients or clients they serve.
FAQs
Q. What is the 5S and how is it related to resourcefulness in the workplace?
A. The 5S is a method for workplace organization and it is not solely dependent on the resources you have. Even with fewer resources, it is about arranging them in a way that they serve you better, making your work environment more productive.
Q. What is the difference between 5S in healthcare and industrial 5S?
A. While both healthcare and industrial 5S share similar principles, the difference lies in their application because of the differences in the industries they are used in.
Q.What measures should a quality professional choose for analysis?
A.Quality professionals should have skills in working with different types of measures, including outcome measures & process measures, to move the needle on processes and influence the outcome measure.
Q.How can 5S and quality be implemented in a countryside healthcare system with monetary constraints?
A. Starting with what resources are available and removing waste from the system is the first step to implementing 5S and quality in a countryside healthcare system with monetary constraints.
Q. What are the potential threats to effective QIP and how can they be overcome?
A. A lack of leadership buy-in is the first potential threat to effective QIP. A clear vision and leadership support are essential for the success of a quality improvement program.

Author
-

Programme director, Safety and Improvement; Director and Improvement Advisor, Institute for Healthcare Improvement